Value-Based Care is the Future of Healthcare Reimbursement.
Value-based care is officially the future of healthcare reimbursement. Systems4PT is the premier EMR in supporting your current participation in this payment model or easily transitioning you into this payment model. Our clinics participate in the federal Quality Payment Program (QPP) through the Merit-based Incentive Payment System (MIPS). S4PT is proactively establishing the necessary integration to make participation in MIPS Value Pathways (MVPs) available to our clinics when they become available to physical therapists.
Patient Data at Your Fingertips
Through the Patient Portal, each patient receives a link to a secure site where they answer specific questions regarding their medical history and complete a Functional Outcome Test (FOT), selected specifically for them. Security measures in place ensure that there is no HIPAA-protected information being exchanged so there is no vulnerability risk to the patient or clinic.
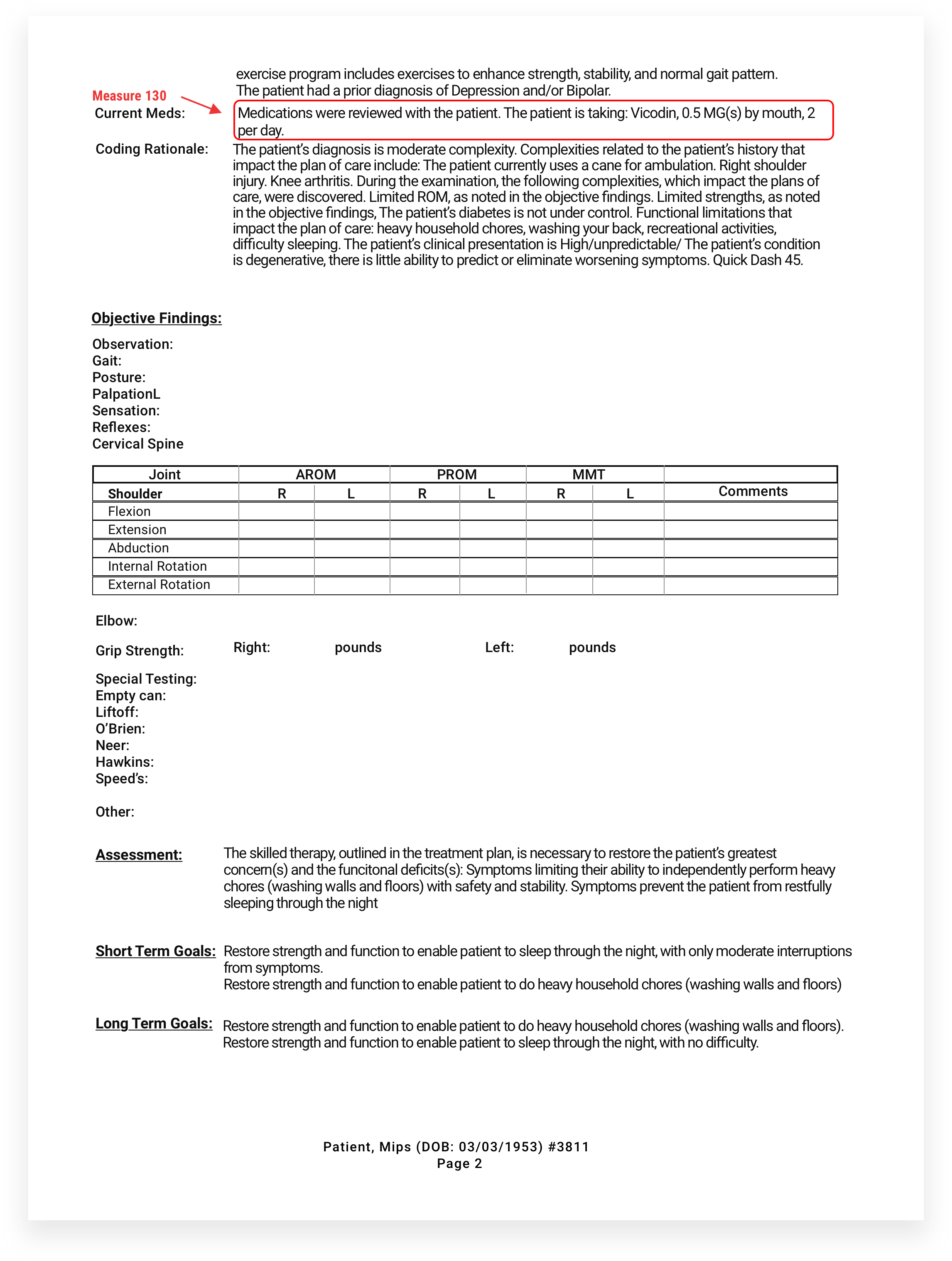
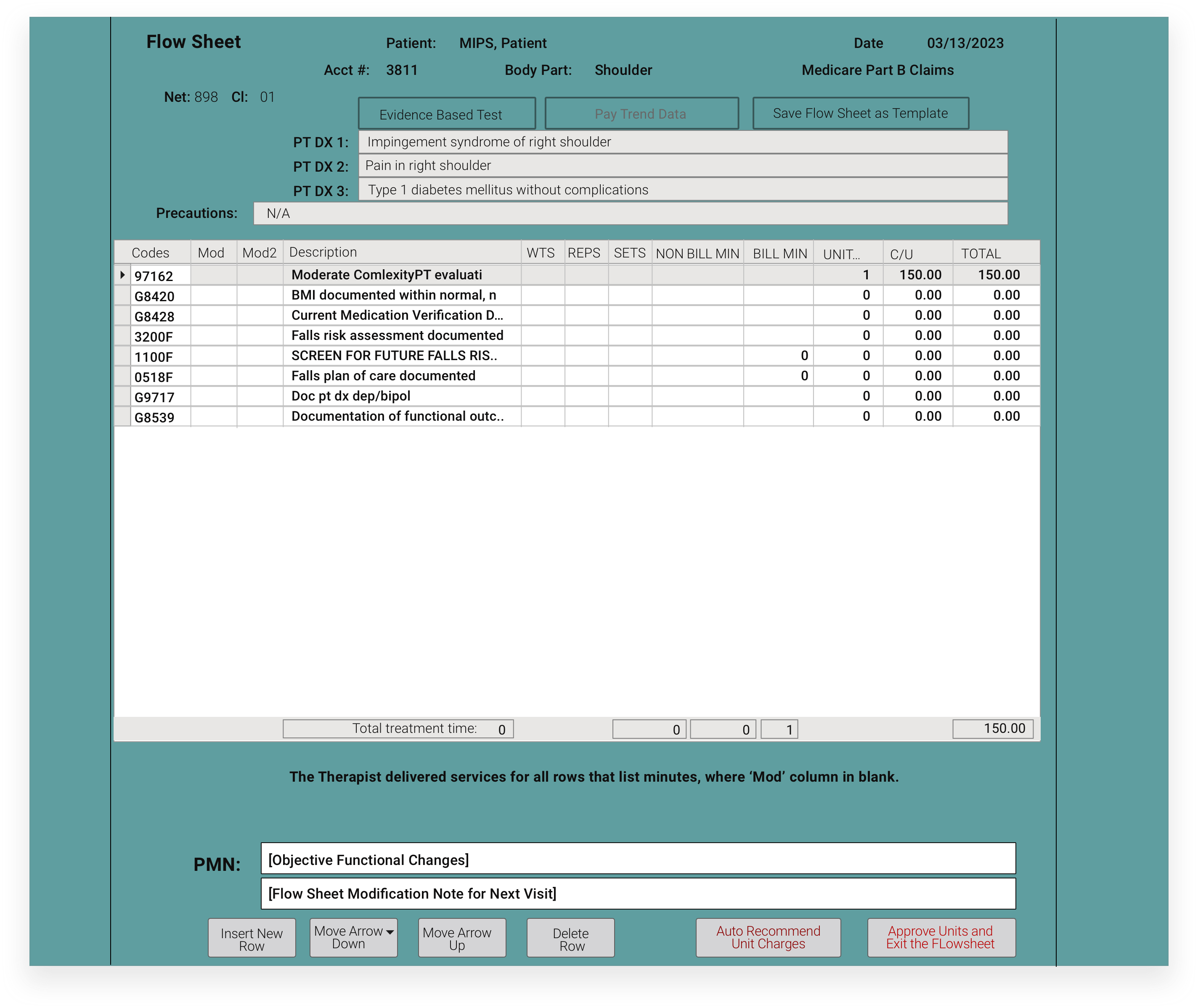
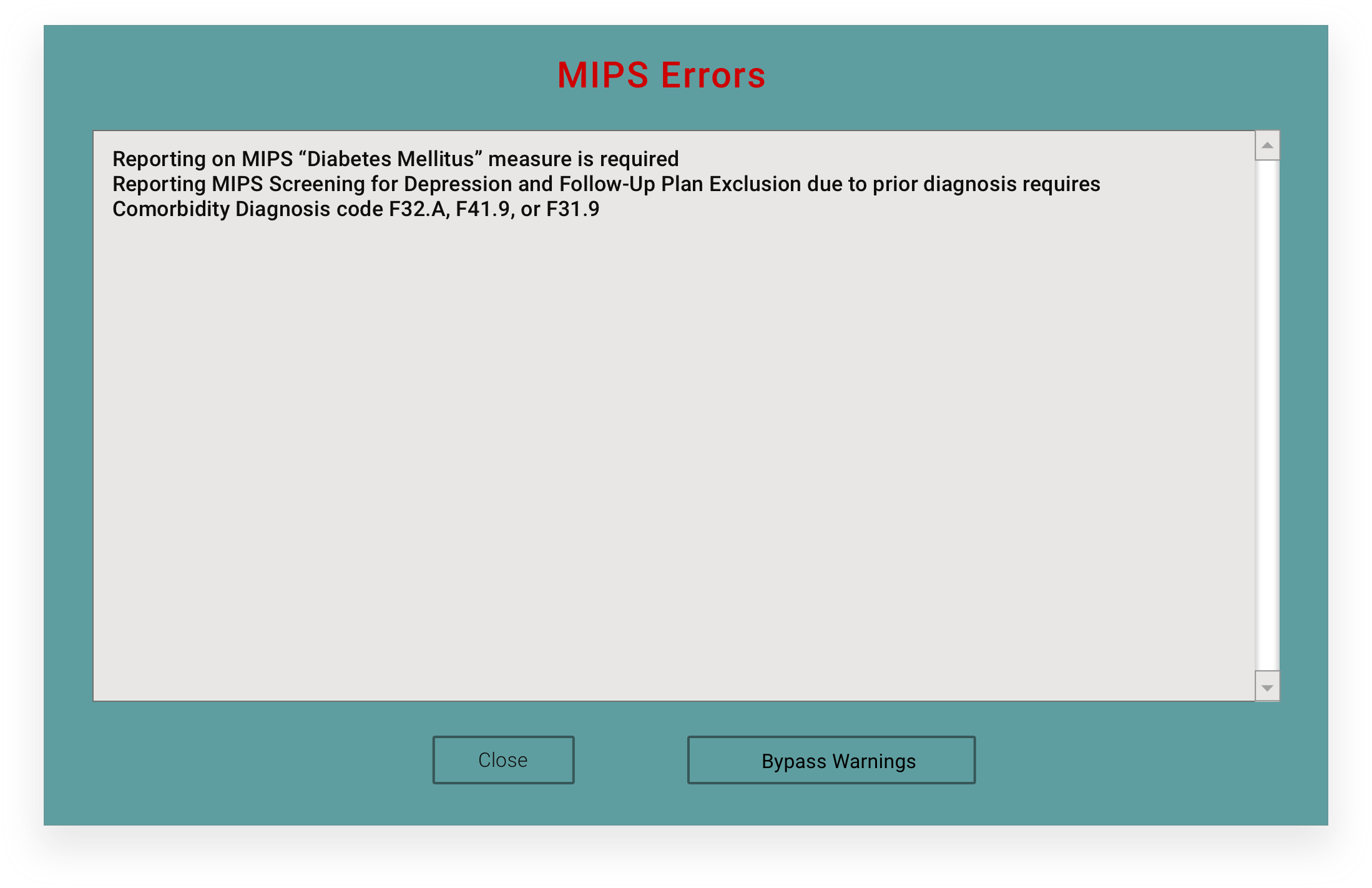
Everything highlighted in red is required documentation for successful MIPS reporting. It was all harvested from the information the patient provided via the Patient Portal and automatically documented in your initial evaluation. All you need to do is read, review with patient, and correct any incorrect information. The software prompts you to complete any other required steps for MIPS.
The EBM will ask you to confirm you want to report the recommended MIPS codes. Once checked, they will appear in your Treatment plan
Additionally, S4PT takes care of the 2 high-value Improvement Activities (IA) required for physical therapists’ successful participation in MIPS. By utilizing the FOT on initial evaluation and progress notes, you meet the requirements for IA_AHE_3, Promoting Use of Patient-Reported Outcome Tools. To meet IA_BE_6, Regularly Assess Patient Experience of Care, and Follow Up on Findings, S4PT automatically sends your clients Net Promoter Score (NPS) surveys, collates the responses, and sends you quarterly reports. Finally, you review the results, document that review as well as any changes you may make based on the results.
Thanks to S4PT’s focus on Medicare compliance and participation in the QPP, many of our clinics achieved the top positive payment adjustment of 8.25% in data collection year 2023. These clinics will be reaping the benefits in 2024!
This year S4PT is collecting and reporting new QCDR measures Lmbr 1 – Lmbr 10 for our clinics. These measures are the key and future of participation in Value-Based Care (VBC) for physical therapists. S4PT is proactive in monitoring and accommodating the future of VBC. Our clinics are ready for this payment model!